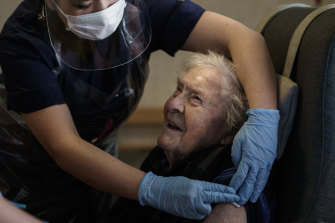
Medical teams will be sent to aged care homes to vaccinate almost 500,000 residents and staff under a federal plan to deliver the jabs outside hospitals and major hubs.
The Morrison government has opened talks with medical companies to set up a “surge workforce” that will fan out to thousands of aged care homes as soon as the Pfizer vaccine becomes available.
The plan takes federal responsibility for delivering help to the sector after costly mistakes between federal and state authorities last year.Credit:Getty Images
The teams will have up to five days to transport the Pfizer vaccine in standard refrigeration to ensure “safe and stable” distribution beyond the deep-freeze storage centres that must store it at minus 70 degrees.
The plan takes federal responsibility for delivering help to the sector after costly mistakes between federal and state authorities last year, when 678 people died from COVID-19 in residential aged care.
Aged Care Minister Richard Colbeck, the subject of fierce criticism last year over the coronavirus death toll, has held briefings with the sector on the appointment of companies to offer the new workforce.
“As far as I’m concerned, the first people who should get the vaccine are the most vulnerable, and they are the people in residential aged care,” Senator Colbeck said on Wednesday.
Volunteers at aged care homes will be included in the program alongside residents and staff.
The new model, called “in-reach” in talks between the government and the sector, means aged care workers and residents will not need to be bussed to vaccination centres despite the storage challenges with the Pfizer vaccine.
Asked about the logistics, the Health Department said the Pfizer vaccine had to be stored between minus 80 and minus 60 degrees prior to thawing.
“Once thawed, the Pfizer vaccine can be stored between 2 to 8 degrees Celsius for up to five days, allowing for safe and stable distribution of the Pfizer vaccine at these higher temperatures where required,” a department spokesperson said.
Health and Ageing Minister Greg Hunt said last week he expected the Pfizer rollout to use between 30 and 50 hospital hubs.
The AstraZeneca vaccine, which is to be manufactured by CSL in Melbourne as part of a global rollout, can be distributed to GP clinics, pharmacies and thousands of other locations because it does not require super-cool storage.
NSW will have Pfizer vaccine hubs at the Royal Prince Alfred, Westmead and Liverpool hospitals, followed by Hornsby, St George, Nepean, Newcastle, Wollongong, Coffs Harbour, Dubbo and Wagga Wagga hospitals.
The Queensland government is setting up six hubs, with two in Brisbane and one each in Cairns, Townsville, the Sunshine Coast and the Gold Coast.
The Victorian government is setting up hubs in the Austin, Western and Monash health services in Melbourne, as well as planning six regional centres in Ballarat, Bendigo, Geelong, Albury-Wodonga, Sale and the Latrobe Valley.
Canberra Hospital in Garran is the hub for the Australian Capital Territory.
The Health Department confirmed the federal plan to this masthead in response to questions about the logistics.
“The Commonwealth will be responsible for the delivery of COVID-19 vaccines to the residential aged care facility sites,” the department said.
“The Commonwealth’s procured surge workforce will prepare and administer the COVID-19 vaccine directly at a residential aged care facility to residents and workers.”
Companies such as Aspen Medical, Healthcare Australia, International SOS and Sonic Clinical Services could be hired to provide the surge workforce and conduct the vaccinations in aged care homes but the federal contracts are yet to be finalised.
The federal plan assumes 217,000 aged care residents, 250,000 staff and about 60,000 volunteers.
All are in Phase 1A of the vaccine rollout, which also includes quarantine workers and front-line healthcare workers.
Older Australians outside aged care homes, including those in retirement villages, are expected to go to GPs and clinics as they would with the annual flu vaccine. This group, called 1B, includes anyone over the age of 70.
Everyone will need two jabs of the vaccine, whether it is from Pfizer or AstraZeneca, with three weeks between jabs. People will need to wait one month before having the annual flu vaccine.
Aged & Community Services Australia chief Pat Sparrow said the in-reach plan was a “good approach” and the industry was working through the details with the government.
Council on the Ageing chief Ian Yates also backed the plan and said the government was consulting on the communications strategy to overcome “anti-vaxxer” scare campaigns against the program.
Vaccinations will take place only after the teams make clinical assessments about each individual, a key issue given the questions over whether very old and infirm people should take the vaccines.
Australia had no active COVID-19 cases in aged care in the last weekly update, released on January 22. There have been 2029 cases among residents during the pandemic so far, leading to 678 deaths, and 2227 cases among staff, all of whom recovered.
Get our Coronavirus Update newsletter
Stay across the news you need to know related to the pandemic. Sent Monday and Thursday. Sign up here.
Most Viewed in Politics
Source: Read Full Article