For our free coronavirus pandemic coverage, learn more here.
I’m relaxed now because I just got an email about an hour ago – we are closing the COVID ward for the time being, so you are off the roster. Seems like the virus is abating – for now. We’ll see. Wasn’t like that a month ago:
It’s Sunday night and I’m about to go to bed. I know I will not sleep well. Because I have been reading. There’s a long technical name for what I have been reading, but the lay version is “How to look after people who are in hospital because they have COVID-19 and not enough oxygen in their bloodstream”.
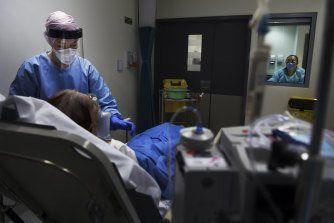
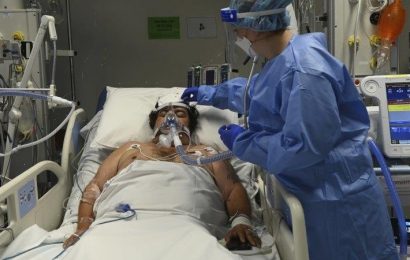
Some of Sydney’s COVID wards have shut – for now.Credit:Kate Geraghty
New stuff for me and I’m learning quickly. The reason I am doing this is that at my hospital there is a lot of COVID. So much so that we have essentially run out of respiratory and infectious diseases specialists. So a dusty old cancer specialist is going to call the shots in a COVID ward.
I get up in the morning, feeling initially liberated because I can get into jeans and a T-shirt. No ironed shirt, pants and tie for me this week. I drive off not listening to Fran Kelly as I start to catastrophise about what might be before me. It will be fine, I tell myself. So, terrified.
I grab some scrubs and beep myself into a room where I change and panic about putting my phone in a ziplock bag. It’s so I don’t infect myself after getting out of a patient’s room – but will the damn thing still work? What about the fingerprint recognition palaver? (Answer: yes, it all works surprisingly well.) Then the P95 mask and goggles.
The masks: mandatory on all wards due to COVID. You have to do this fit-testing, where they work out which one is right for you, doesn’t leak or let stuff in. For me, it was the “duck-billed” mask. Actually, more comfortable than the others. But I had a patient who decided to call me Donald all the time. Thought it was hilarious. Again and again, she laughed. So perhaps slightly good that I’m now in the COVID ward and no one laughs.
No one laughs. Bloody hell. These are really sick people. Everyone is on oxygen, there is coughing, spluttering, body aches. When I finally get into a room (gowned, gloved, goggles and visor on), I’m looking at a terrified person who has never seen me before and, I realise, doesn’t speak much English. Reassuring body language is hard. “I’m the doctor!” “You’re going to be all right!” Not that I actually know that. I do some gloved shoulder-squeezing to reassure, listen to the chest, feel the tummy and get out of there. You’re supposed to limit the time you are in the room.
And getting out of there isn’t easy – you have to gradually divest yourself of all the clobber you are wearing without touching anything. A kind of bizarre ballet without the music.
As it turns out, the clinical care is intensive but not that complicated. The infectious diseases team have done a spectacular job of codifying everything for us. There’s a bunch of drugs that help (NOT ivermectin, Donald and Craig) and criteria for when to use. I had a pregnant 30-year-old. “Don’t use A, use B,” said the daily updated guidelines, so that’s what we did. (Should I have asked Clive Palmer?)
As well, we now have a very low tech but very well-proven strategy to prevent the need for artificial ventilation and reduce the chance of dying: turn people on their fronts. Sounds crazy but actually makes sense. We don’t normally do CT scans on these patients because it doesn’t really help. However, sometimes we need to (for example when there might be a blood clot). And when you look at these scans it’s amazing. All the disease is at the back: blood is going through there and picking up zero oxygen. Turn them over and suddenly the oxygen levels rise. I’ve seen it happen in minutes.
It’s not until mid-afternoon on my first day that I notice a clear sunny sky outside. I need to sit down and eat something. From the ninth floor of the new hospital building, I can see Centrepoint Tower from one end of the ward and the Blue Mountains from the other. I’m seeing my city, home to 5 million people. I spend a few moments breathing in some peace and normality. I’m liking that I have helped (I know only a little bit) my town.
So that was seven days for me last month. I went back to my job as a cancer specialist. Things have kind of got back to normal.
However, I find myself reflecting on the systems I was part of without really realising it. For a start, there was the frightening realisation that we didn’t have enough doctors and nurses to run the COVID show. There was massive rearrangement of rosters. In my own little world, suddenly our ward registrars were taken off the cancer ward and put on COVID wards. Our specialist registrars also went off to the COVID wards (and helped me not look like an idiot when I was there).
I never heard someone say they wouldn’t help.
Can we please remember this? That public medicine is a triumph.
Nicholas Wilcken is a Sydney-based oncologist.
The Opinion newsletter is a weekly wrap of views that will challenge, champion and inform your own. Sign up here.
Most Viewed in National
From our partners
Source: Read Full Article